Vertebroplasty Research studies
Vertebroplasty Research studies / treatment.. This is a medical treatment that addresses the treat pain and spinal curvature caused by Osteoporosis fractures of the spine.This page offers information from scientific research papers about the effectiveness of this treatment.
If you are looking for a description of the treatment - what is is and how it is done, then you should go to the page that described this Surgical treatment for Osteopososic back hump
Background and Vertebroplasty research studies - the results
The first time this procedure was performed was in 1984 by Gakibert and Deramond, in Amiens, France. Since that time, there have been more surgeries and so many more experienced practitioners.
Experience is important. If you are considering this procedure, do ask the surgeon how many of these procedures he or she has done.....and what the outcomes have been.
During this procedure there is an injection of bone cement into the cancellous or spongy tissue of the vertebra "to alleviate pain associated with compression fractures, prevent further loss of vertebral height, and correct . . . deformity."
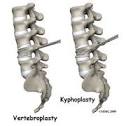
In follow up studies of both the proceudres to relieve back hump, pain relief was a major outcome. (vertebroplasty, 87%; kyphoplasty, 92%). Both procedures showed similar spinal height gains. Back hump was significantly alleviated. These procedures offer hope for a better quality of life to you if you have been suffering from curved spine due to osteoporosic fractures.
If you are considering this procedure, you might want to ask why your physician is recommending it (as opposed to Kyphoplasty)
Frequently asked questions
1. Given the fact that most persons undergoing the procedure are older, some ask, " Am I more likely to suffer a stroke after this operation?" The answer is NO.
Iin 2012 researchers Ching-Lan Wu, Jau-Ching Wu, [...], and Cheng-Yen Chang published an article, The Risk of Stroke after Percutaneous Vertebroplasty for Osteoporosis: A Population-Based Cohort Study, that showed patients who underwent this procedure were no more likely to have a stroke than those who did not have the procedure. And that is good news.
2, Are there risks of negative side effects during or after this procedure? The answer is YES.
a.Sometimes there is "cement leakage, cement embolism, pulmonary embolism, hematoma, neuro decline, spinal cord compression, radiculopathy, infection, and adjacent vertebral fracture".
b. If there is leakage into the venous channel, life threatening conditions such as pulmonary embolisms can occur.
c. Sometimes adjacent vertebra may fracture post-operatively. This would be a serious and discouraging event.
Conclusion: If you are considering undergoing this procedure , be sure to discuss the possibility of some negative outcomes with your surgeon BEFORE undergoing treatment. All have been reported in the research studies and so your surgeon ought to be prepared to discuss them with you.
Click to read the complete Vertobroplasty research studies article cited on this page.
Read about other treatments for back hump:
- Kyphoplasty
- Taping of the back to relieve curvature
- Special exercises

